Otoplasty
Conveniently located to serve the areas of New York, NY
An otoplasty is is an operation that improves the cosmetic appearance of the ears. Abnormalities of shape, size, and projection may be corrected during this type of operation. Historically, there have been many techniques described for the cosmetic repair of numerous congenital probelms. They have evolved from cartilage cutting, folding, and suturing to create the look of a normally developed ear.
The correction of prominent ears, also known as “ear pinning”, is the most common type of otoplasty designed to reduce the prominence of the upper portion, the antihelix, and the height of the concha, the surrounding opening of the ears. The procedure can permanently correct ear positioning, preventing them from projecting too far outward from the scalp.
If you are embarrassed about your own ears, or if you have a child who has been feeling self-conscious about their ears, a relatively simple otoplasty procedure can work wonders for overall facial harmony. For many children, especially, abnormally developed ears can be a cause for ridicule and bullying. Adults may feel the need to cover their prominent ears with long hair or hats.
With the highly advanced and minimally invasive techniques of Dr. Sherman, you can achieve a renewed sense of confidence in your appearance. Dr. Sherman is an award-winning doctor with decades of experience performing both plastic and reconstructive surgeries. As a senior plastic surgeon at Cornell and a leader in his field, he takes extra care to stay up-to-date regarding the latest research of every procedure he performs. To see if his otoplasty surgery is right for you, call his practice in NYC at (212) 535-2300 or inquire with his contact form.
“I recently had an otoplasty procedure. A lot of people had been laughing at my ears but Dr. Sherman fixed that for me. I’m nine years old. He also invented tools that he uses in all the procedures. My ears look outstanding!! He is a #1 doctor and a spectacular surgeon!!!! Thank you Dr. SHERMAN!!!!!!!!!!!!”
Otoplasty Patient
Contents
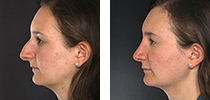
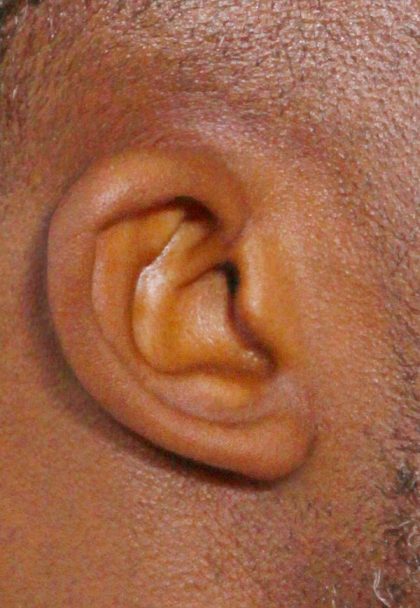
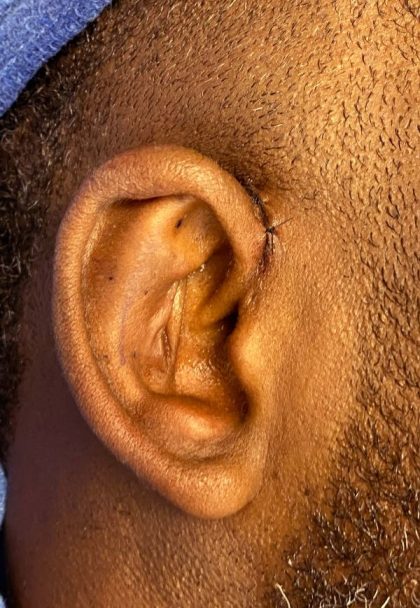
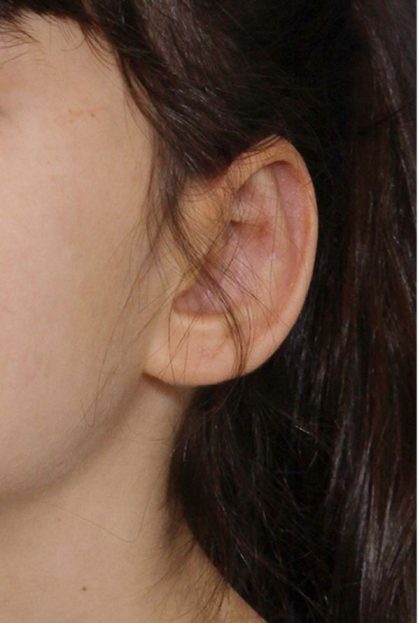
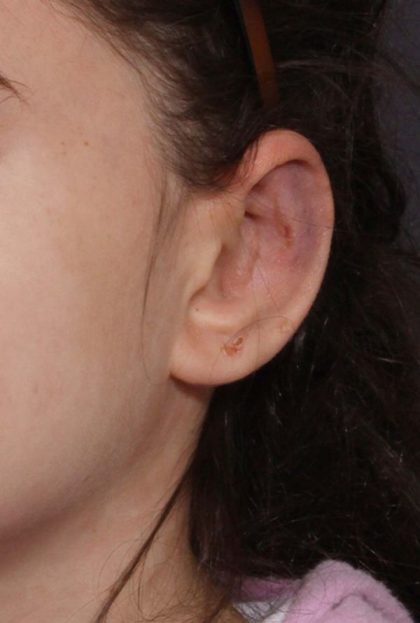
Before and After Photos
About the Otoplasty Procedure
According to statistics from the American Society of Plastic Surgeons, surgeons performed 53,095 otoplasty procedures in 2020. (1) In the realm of cosmetic surgery, it is not hugely popular, but within Dr. Sherman’s office, it is one of the most highly-requested procedures.
At birth, the outer cartilage structures of the ears are roughly 52 to 75% of their adult size and quickly mature during the first few years of life. (2) This makes the otoplasty safe enough for children since the ears are one of the first structures to fully develop at a young age. We can often perform surgery on children as young as 5 or 6. Prominent ears are most commonly caused by an autosomal dominant trait inherited from family members- if you have them, chances are that other family members have them as well. The condition may be bilateral (both ears) or unilateral (only affecting one ear).
Dr. Sherman can custom tailor his otoplasty procedure to promote symmetry between the ears, even if only one is affected.
The Structural Difference in Prominent Ears
Prominent ears stick outward from the scalp due to one main issue- the flattened appearance of the upper outer antihelix. In a normal ear, the antihelix has a Y-shaped fold, dividing the upper ear into two segments: the superior and inferior crus. Because of this abnormality, the ear lobe may be angled more outward and the concha may also be significantly deeper. For an otoplasty, Dr. Sherman can recreate the Y-shaped fold and decrease the height of the concha to make it appear less noticeable. These changes also help rotate the ear lobe inward.
Dr. Sherman has created a video that is available on YouTube. Part one describes the anatomy of the prominent ear, part two describes the surgery and shows it in detail, and part three shows the end result. This set of video instructions has served as a teaching tool for residents and plastic surgeons alike. They have gained over 100,000 views on YouTube.
Candidates for Otoplasty
Ideal candidates are over the age of 5 and without any blood-clotting disorders or conditions that could affect the recovery process. They should be in good overall health and have realistic expectations for the procedure. Normally-developed ears do not sit flat against the scalp, so Dr. Sherman will not create this kind of result. Finally, adult patients should be non-smokers or able to quit for a period of a few weeks to promote optimal healing.
Personal Consultation
During your consultation with Dr. Sherman, you will be able to discuss your concerns about the procedure and gain valuable insight into how it works. He will evaluate the aesthetics of your ears and inquire about the results you would like to see. As a highly experienced surgeon who has been featured in magazines and the Today Show for his expertise in otoplasties, Dr. Sherman utilizes the most effective methods possible that have left thousands of patients pleased with their outcomes.
If you feel ready to take the next step today, get in contact with his practice in New York City by calling (212) 535-2300 or by filling out our online form, and a member of our staff will schedule your appointment.
How to Prepare
Dr. Sherman will perform blood tests for patients over the age of 50. For younger patients, if the procedure is performed under local anesthesia, no tests are needed as long the proper medical history is taken. If older patients choose sedation, medical clearance must be sought. If you smoke or consume other forms of nicotine, you should aim to stop for a few weeks to promote better blood circulation. Dr. Sherman will review your medications and supplements and provide you with guidance on which ones to refrain from taking.
Procedure Steps for the Otoplasty
Dr. Sherman takes a different surgical approache for each patient, depending on their unique cosmetic needs. Firstly, his anesthesiologist will place you under general anesthesia, or he will administer sedation with local anesthesia. From there, he will make a small incision in the back of the ear to access the outer cartilage. He will place internal sutures in the cartilage, recreating a more normal-shaped upper ear area and realigning the placement of the ear lobe. He will do the same to the other ear where required. The entire procedure will take just under 2 hours.
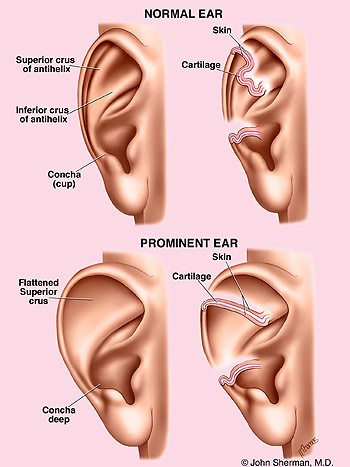
The top left illustration shows the anatomy of a normal ear with the proper development of the inferior and superior crus, and normal contour. The upper right illustration shows a normal folding of the cartilage that must be replicated during ear surgery.
The lower left illustration shows the flattening of the ( SCAPHA) without the formation of the superior crus of the antihelix. Note on the cross-section the lack of folding.
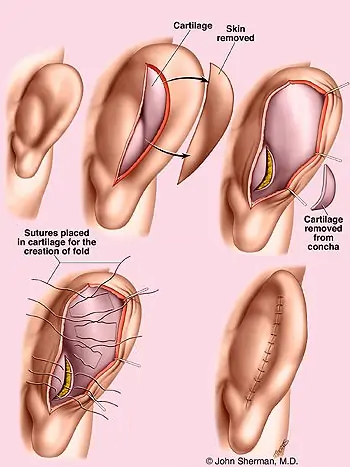
These illustrations show the sequence of the repair. The entire repair may be performed either from behind the ear (posterior) or in some examples from the front. An ellipse of skin is removed from behind the ear allowing access to both the concha and the area of the folds that must be re-created. The second illustration on top shows the removal of the concha which reduces the size of the concha and allows access to the front of the ear for recreation of the folds. The lower row of illustrations shows the sequential placement of internal sutures (Mustarde) that re-creates the folds, and additional sutures to reduce the size of the concha.
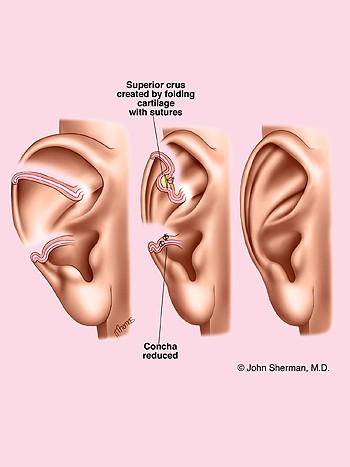
This last panel shows the preoperative ear with a lack of folding and the placement of the sutures that re-create the fold and reduce the size of the scapha.
Recovery and Results
Though you will be able to go home on the same day of your procedure, keep in mind that you will still be uncomfortable, swollen, and slightly bruised for a few days. You should take care to avoid any over-the-counter medications that could thin the blood and create more bruising. At around the 4 or 5-day mark, you will have to return to Dr. Sherman’s office for bandage removal and a quick evaluation of your healing.
After your bandages are removed, it’s important that you use a headband that will protect your incisions if you happen to sleep on your side. Dr. Sherman encourages patients to use this band for the first month to ensure the contours of the ears aren’t negatively affected. At the 10-day mark, he will remove your external sutures. Usually, by this point, the bruising has completely subsided. It takes roughly 2 to 3 weeks before you will get to enjoy your final results.
Corresponding & Complementary Procedures
Ear Reduction
It is possible to have both prominent and enlarged ears, two cosmetic issues that Dr. Sherman can resolve. To treat this condition, called macrotia, he will recommend an ear reduction in which he will remove excess cartilage to form smaller outer ear structures that are more flattering to your particular face shape.
Stahl’s Ear Correction
If your ears have a pointier appearance at the tips, you could benefit from a Stahl’s ear correction, another procedure that involves modifying cartilage. For this surgery, Dr. Sherman will fashion the helical rim into a more typical rounded shape. If necessary, he can also create a natural-looking fold at the top corner of the helical rim for patients who lack this feature. Dr. Sherman can perform this type of outer ear correction utilizing just local anesthesia.

Cost of an Otoplasty in New York City

At the time of your consultation, Dr. Sherman will give you a cost estimate for your procedure with surgical fees, medications, anesthesia, etc. taken into consideration. If you have health insurance, you should check with your policy provider to see if otoplasty is covered. There are some insurance policies that reimburse the cost of the otoplasty operation if performed in the early childhood years. This is not a common occurrence, so we offer financing options for our patients. Our office staff will help you contact your carrier to see if this may apply to you. Schedule a consultation at our office today, or give us a call at (212) 535-2300 to find out more about Dr. Sherman’s unique approach to otoplasty. To learn more about other procedures, browse through his website’s blog.
FAQ
What is the minimum age requirement for an otoplasty?
Otoplasty is suitable for healthy patients over the age of 5.
Are there any possible complications of ear reshaping surgery?
The incidence of complications stemming from otoplasty are remarkably low. Occasionally, patients require a correction since the original sutures may not hold and the original protrusion can redevelop. The younger the patient, the less chance that this will occur.
Will I have scars after an otoplasty procedure?
You will have some scarring after the procedure, but it will be on the back side of the ears. After a few weeks have passed, scarring will diminish significantly and appear less red and irritated.
References
- American Society of Plastic Surgeons. Plastic Surgery Statistics Report.; 2020. https://www.plasticsurgery.org/documents/News/Statistics/2020/plastic-surgery-statistics-report-2020.pdf
- Purkait R. Progression of Growth in the External Ear from Birth to Maturity: A 2-Year Follow-Up Study in India. Aesthetic Plastic Surgery. 2013;37(3):605-616. doi:https://doi.org/10.1007/s00266-013-0097-1